Possible Causes
What Causes Fibromyalgia?
& Why So Many Symptoms

Fibromyalgia consists of a slew of malfunctions, most of them hidden away in the central nervous system (spinal cord and brain) or CNS. No obvious signs of injury or disease exist, but there are several less conspicuous abnormalities throughout your body. And despite hurting from head to toe, lab tests are usually normal. Researchers don’t know what causes your fibromyalgia symptoms, but genetics or heredity plays a key role.
Fibromyalgia patients rarely claim, “I was born feeling this awful.” Instead, their symptoms surface later in life despite genetic predisposition to developing fibromyalgia. Researchers believe the disease onset is triggered by an event or threat to the body. Common examples include infection, injury, trauma, or another disease such as rheumatoid arthritis. These events disrupt the pain processing system, but it’s only supposed to be temporary.
In genetically predisposed people with fibromyalgia, things go haywire and chronic widespread pain develops. In turn, the mishaps in the CNS set off a snowstorm of changes that cause fibromyalgia symptoms to appear. Making matters worse, other body systems respond by wreaking havoc everywhere.
Pain normally serves a protective role, forcing you to take it easy so your damaged tissues heal. It’s a danger signal that prevents you from risking further injury. Yet the chronic pain of fibromyalgia has long outlived its purpose, resulting in a disease of the CNS as well as the peripheral systems that communicate with it.
Where is Your Pain?
Even if all your muscles feel wrenched, your pain does not actually occur there. Instead, biochemical changes in your muscles are picked up by your neurons, which transmit signals to your brain. Then it’s your brain (not your muscles) that perceives the signals as painful.
Distinguishing between where injury or disease occurs and how pain is perceived is essential for explaining what causes the widespread discomfort of fibromyalgia. Otherwise, if one thinks that the source of pain must be in the tissues felt to be “painful,” one can clearly become suspicious when tissue abnormalities aren’t found. In turn, this leads to the false assumption that your pain is of psychological origin.
To understand an abnormal pain state like fibromyalgia, you need to know what’s considered “normal.” The next section takes you through the Cliff Notes version of what should happen if you merely stubbed your big toe.
Pain Control Simplified
Jamming your toe hurts, but the soreness disappears in days if your pain circuitry works. Chemicals are released in the injured toe, activating sensory nerve fibers that send signals to the spinal cord. After a few relay stations, the signals reach the brain where they are interpreted as pain localized to the toe.
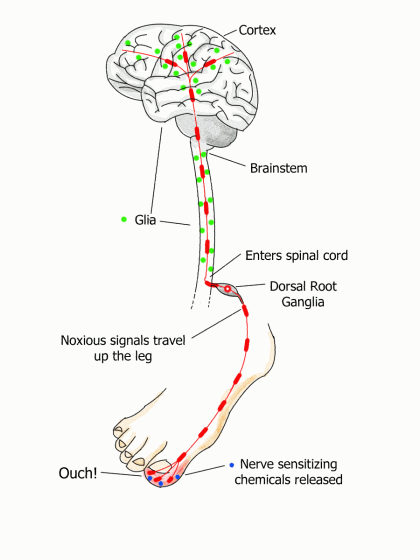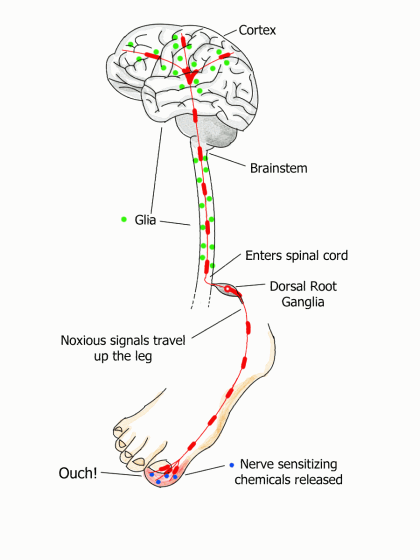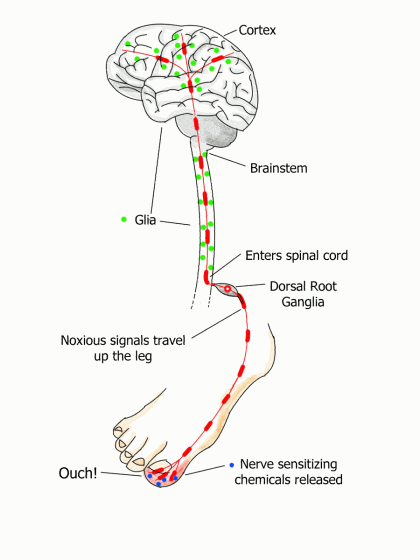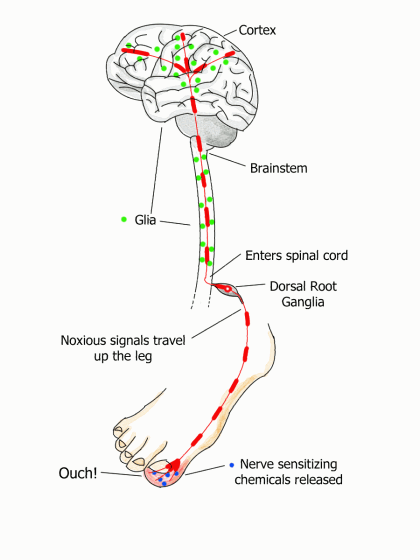
The communication highway from the toe to the brain has checkpoints surrounded by immune cells called glia. Ordinarily, these cells nurture the neurons and survey the environment for any threat, such as an injury. When the toe is stubbed, your glia pour out substances to sensitize nerve endings. This makes them fire off more alarms to get your brain’s attention. Below is the three-step process that follows a stubbed toe.
- The tentacle-like endings of sensory nerves pick up chemical changes in your sore toe and start generating noxious signals that travel up the leg to the spinal cord. Just before these transmissions enter the cord, they pass through a bulb-shaped structure called the dorsal root ganglia. The ganglia house the control center or nucleus for each neuron that passes through it. They are located at every level of your spine on both your right and left sides. (These ganglia can decrease or increase the signal, and researchers suspect they are doing the latter in fibromyalgia.)
- The noxious signals connect with neurons just inside the spinal cord. Your spinal neurons release opioids and other pain-relieving substances to dull the pain. In addition, your glia morph into an activated state, causing the release of substances that temporarily sensitize the sensory neurons. It’s a mechanism to bolster the signal to get your brain’s attention.
- Once the signal travels up the spine, it connects with the neuron/glia checkpoints in the brainstem (base of brain). After the signal reaches the cortex, more pain-relieving processes are triggered.
If everything works properly and you protect your foot with the injured toe, the noxious inputs to your CNS stop. Your glia become mellow and the pain goes away. But in fibromyalgia, the triggering event (more than a stubbed toe) doesn’t resolve and the glia remain active. As a result, you are left with chronic fibromyalgia pain and your genetics are likely to be blamed.
Role of Genetics
First degree blood relatives of fibromyalgia patients are 8.5 times more likely to develop this condition.1 Looking at just siblings, if a brother or sister has this disease, the chance of other siblings developing it is one in four. 2 Overall, the risk of fibromyalgia surfacing appears governed by a fifty-fifty combination of genetics and the triggering event. Of course, this is just a guess.
Genetic alterations in the body’s production of pain-relieving chemicals tend to occur more commonly in fibromyalgia. For example, researchers identified differences in serotonin and dopamine production as well as changes in the way opioids work. However, each abnormality only occurs in a subset of patients and others will likely be found. These genetic changes explain the variability in symptoms, but no one culprit appears to cause fibromyalgia.
Brain Transformations
Is there something about your genetics that makes you more vulnerable to developing fibromyalgia? A large-scale brain imaging study following 300 children (9-10 years old) over a one-year period offers answers.3 All were pain-free to begin with, but the children who later developed pain displayed alterations in the way their brains operated. In fact, the youngsters who experienced pain in multiple regions just one year later showed transformations in brain function that parallels adults with fibromyalgia.

All too often, patients are told that depression or anxiety causes their fibromyalgia pain and other symptoms. But Daniel Clauw, M.D., of the University of Michigan and researcher on the above study in children set the record straight:4
“The depression appears years after the development of widespread pain, rather than causing it. The same holds true for pain catastrophizing” (e.g., symptoms of anxiety). “The sleep disorder comes first, followed by memory problems, pain, and then finally, depression.”
The study in children reveals that the fibromyalgia brain is genetically predisposed to function abnormally. However, there are many contributing factors in the central nervous system (CNS). The problem could be at the level of the spinal cord, the brainstem, or the brain. Alternatively, defects at all three levels of processing the incoming signals may exist. Then there are the glia and numerous chemical messengers used by your neurons (transmitters). Several are increased fourfold in the CNS while others are nearly depleted. And don’t forget about sleep. It plays a role in orchestrating many brain functions.
Driving Forces
Does your brain cause other systems in your body (out in the periphery) to malfunction, or does one of these other systems set off your brain alterations? This is an ongoing debate among researchers. After all, there is a two-way communication network between your CNS and the rest of your body.
Hypothetically, if a peripheral system is the driving force behind your fibromyalgia, what are some likely candidates? Three possibilities include your immune, gastrointestinal, and autonomic systems … and there are others. In fact, research shows you have an intense amount of pressure inside your muscles that make them hurt. In turn, this sends more signals to scramble your CNS.
Immune system components in the blood can cause the dorsal root ganglia to ramp up the transmissions entering the cord. Over time, the CNS becomes overloaded and the brain doesn’t work properly. The immune system changes in fibromyalgia are subtle and likely tied to genetics.
Your gastrointestinal (GI) system does so much more than digest food. It has a direct line of communication with the brain (and vice versa) and it is disrupted in fibromyalgia.5 Again, the GI abnormalities are probably linked to your genetics.
Communications between your CNS and all your peripheral organs are transmitted through your autonomic nervous system. This system isn’t operating correctly in fibromyalgia and causes many of your symptoms.6 But given the strong CNS-autonomic connection, it’s unclear which is the chicken and which is the egg.
High Variability

When researchers claim an abnormality is more prevalent in fibromyalgia patients, it doesn’t mean every patient has this defect. Diffuse widespread pain is the cumulative result of different hiccups in the CNS and peripheral systems. Keep this in mind because it helps explain the variable reaction to treatments.
One person might have an amazing response to a drug, while another may think it is worthless. Both are fibromyalgia patients, but their genetics and the processes contributing to their symptoms can differ.
Many researchers claim fibromyalgia is not a single disease. Instead, they believe the illness is composed of several related diseases (or subgroups) because they can’t find the same abnormality in all patients. Most likely this is because they haven’t uncovered the right abnormality (the one at the epicenter) that ties all fibromyalgia patients together. As a result, treatments just intercept downstream events, which explains their variability and frequent lack of efficacy.
Puzzle Pieces & Treatments
You can’t change your genetics and it’s too late to undo the triggering event that ignited your illness. However, learning about the CNS and peripheral system glitches will help you understand what causes fibromyalgia symptoms and why certain treatments are beneficial.
With so many puzzle pieces connected to your disease, it’s difficult to treat. You can’t just target one or two pieces of the puzzle to get relief. Instead, you and your healthcare providers need to be creative. The fibro beast must be attacked using several different approaches. Below are strategies to tame your symptoms:
CNS Medications – Most try to strengthen your pain inhibitory processes, while LDN mellows out your glia cells. Overall, this prevents your brain from becoming overwhelmed so it can function better. Side effects are often problematic, so ask your doctor about cutting the dose.
Nondrug Therapies & Self-Help – Use these in combination with medications to improve your pain-fighting system.
Treat Muscle Pain – Not only do those painful knots in your muscles hurt, but they also send distress signals to your CNS which overload it. Learn how to interrupt this vicious cycle.
Diet & Staying Fit – Certain dietary ingredients aggravate the CNS and GI systems. Also, prolonged inactivity makes fibromyalgia worse, but too much exercise causes symptom flares.
For simplicity, articles on the Central Nervous System are presented first. It is best to start with Chemical Imbalances and read the articles in the order listed. Pages pertaining to the Peripheral Systems are in the next section.
Treating fibromyalgia shouldn’t be a guessing-game! AFSA funded six projects in 2024 and 2025; help us fund more in 2026.
Stay Current on Treatments & Research News: Sign up for a Free Membership today.
Symptoms | Medications | Alternative Therapies | Muscle Pain Relief | Fibro Friendly Exercises
References for Fibromyalgia Causes
- Arnold LM, et al. Arthritis Rheum 50(3):944-952, 2004. Free Report (read only)
- Arnold LM, et al. Arthritis Rheum 65(4):1122-1128, 2013. Free Report
- Kaplan CM, Clauw DJ, et al. Clin J Pain 39(11):588-594, 2023. Free Report
- Daniel Clauw, M.D., Methodological Approaches to the Study of Widespread Pain and Fibromyalgia, IASP Workshop, August 5, 2024.
- Minerbi A, et al. PAIN 160(11):2589-2602, 2019. Abstract
- Contreras-Merino AM, et al. Int J Psychophysiol 175:61-70, 2022. Free Report
