Fibromyalgia Basics
Clumsy or Off Balance?
– Fibro Research & Therapy Advice

Balance and coordination issues occur in 45 to 65 percent of people with fibromyalgia. In fact, you are six times more likely to fall than a healthy person your age. And this doesn’t include incidents like bumping into walls or end tables. Nor does it capture how awkwardly clumsy you feel at the dinner table, worried that your two left hands will knock over your glass or drop a fork.
Snapshot of Findings
Below are common balance and coordination issues identified by researchers:
- Your body sways when you close your eyes while standing upright. Or you struggle to walk 10 feet with one foot in line with the other (heel to toe). These two neurological tests reveal that 63% of fibromyalgia patients have trouble balancing and 53% have poor coordination.1
- You can only reach forward 11 inches (versus 15 inches for controls) while keeping your heels on the ground.2
- You must reduce your walking speed (30-40%) when navigating on an uneven surface (foam blocks) to avoid wabbling.
- You take 40% longer than healthy people to get up from a chair and walk three meters while subtracting 7s backward from 100. In other words, you slow down coordination of movement (gait) to keep your balance when your attention is divided (counting).
- You require 40% longer than healthy controls to stack four checkers (a test of eye-hand coordination).3
Although strength and flexibility both influence balance, researcher Kim Jones, F.N.P., Ph.D. (now at Emory) says these factors are not the major source of the impairments in fibromyalgia. Patients in her study had strong enough ankle strength to stand on their toes while holding onto a support bar. But when they let go, they could not maintain their balance.
So, what’s causing your lack of coordination? A defect in one or more sensory systems could be tripping you up.
Points of Vulnerability
Your head uses input from your eyes (visual) and ears (vestibular system) to determine its orientation in space. Your trunk’s position is determined by sensors in your neck and sensors in your joints and muscles convey the location of your limbs. Together, your neck controls and muscle/joint sensors comprise your proprioceptive system.
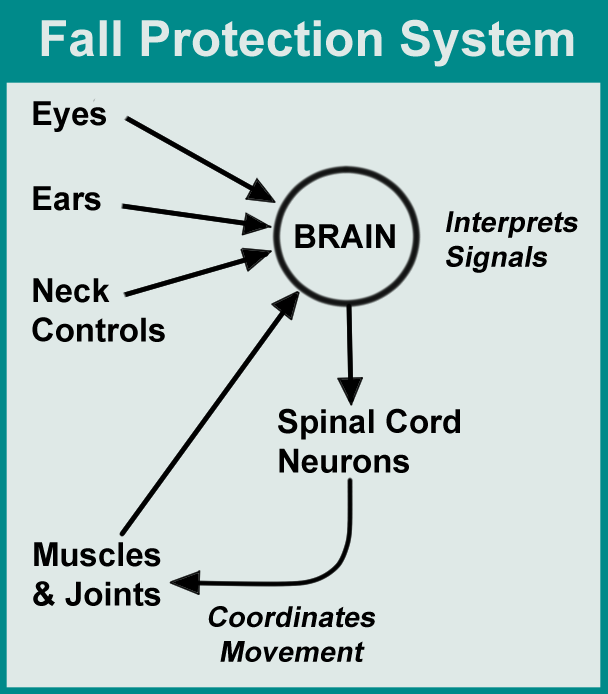
In a nutshell, you have three main sensory systems (visual, vestibular, and proprioceptive) that signal your brain about body positions. But don’t overlook your central nervous system. All three sensory systems form a dialog with your brain and spinal cord to coordinate movement.
All Systems Impaired
Posturography is the gold standard for pinpointing which systems involved in balance are malfunctioning. Subjects stand in an enclosed circular chamber with the platform and the visual surroundings manipulated by a computer.
Your balancing abilities are determined based on how your body responds in the chamber. Can you maintain your upright posture when the platform moves? What about when your eyes are closed? And how about when the visual surroundings are manipulated to make you think you are swaying?
Each scenario forces you to rely upon different sensory systems. For example, when standing on a moving platform blindfolded, your vestibular system keeps you upright.
Jones performed posturography on a group of patients and healthy controls.4 “The balance scores for vestibular, visual and proprioception were significantly impaired in fibromyalgia patients,” says Jones. So, it doesn’t matter which system you depend on for postural stability, none of them work well.5
But what about your brain’s influence on controlling your balance? Jones asked all subjects to complete a questionnaire to assess their cognitive function. No surprise, a decreased ability to balance correlated strongly with reduced cognitive function. Disease severity and being overweight were also related to poorer balance.
“The take home message,” says Jones, “is that the brain/spinal cord must be functioning optimally to make automatic adjustments to maintain balance. Since all systems were impaired, the data suggests that central dysregulation is at the heart of the balance problems in fibromyalgia. If only one system were involved (e.g., the vestibular system in the ears), then we could do very specific interventions to address only that system.”
Other Factors
What do fibromyalgia patients report as the most common situations or symptoms that precede falls or near falls?6 Debra Rose, Ph.D., of Cal-State-Fullerton, asked her patients to keep daily diaries to answer this question. Here’s what she found:
- Falls commonly involved activities that required turning/pivoting or navigating uneven surfaces/steps.
- Patients often reported feeling dizzy just before they almost fell. “Dizziness may serve as a warning signal,” says Rose. Adding, “it allows you time to grab a support to avoid falling.”
Dizziness is reported in 30-80% of patients. It may come and go, but for some patients it’s disruptive. Research links this symptom to a malfunction in the way your brain processes your ear’s vestibular signals.7 Fibromyalgia patients with more distorted signals were more likely to experience dizziness or vertigo (the false sensation of movement), which can throw you off balance.
One more point: the pain itself is not why you are unsteady on your feet. A study comparing people with fibromyalgia and those with chronic low back pain shows your balance issues are more severe.8 Quite possibly, the sensory and cognitive systems are more disrupted in fibromyalgia.
Eye-Hand Coordination
The above studies explain why maintaining an upright posture is difficult, but what about your eye-hand coordination? Arm and hand movements rely on effective communication between the position sensors in your joints/muscles (proprioception) and your brain. And both systems are compromised in fibromyalgia patients.

Compared to age-matched healthy subjects, fibromyalgia patients require significantly more time to perform the following dexterity tests:
- pick up paperclips and put them into the jar
- stack a pile of checkers
- insert nail-sized pegs into a row of holes in a board
- write (copy) a 24-letter sentence
- pick up large heavy objects placed in front of you
The above findings are likely due to abnormal central nervous system controls and explain why you require more time to perform simple everyday movements.3
Balance Therapies
Standard fitness programs often prescribed for fibromyalgia are inadequate for treating balance problems. Remember this when asking your doctor for a physical therapy referral or implementing your own rehab program.
“The program needs to target the specific balance problems identified and challenge the individual in a progressive manner,” says Rose.9 “The emphasis should be on multidirectional weight-shifting and transfer activities while standing or moving in altered sensory environments. For example, with eyes closed, on uneven surfaces (foam blocks), and while turning the head.”
Also learn to find your center (including eyes closed). Next try lifting one foot off the ground (have a support nearby).
The above tasks include different sensory challenges and are important because all systems are impaired. They also help your body adapt its reliance on different sensory inputs to prevent falling. Yoga and tai chi (modified for fibromyalgia) can also help and be more enjoyable than standard balance therapies.
Once your balance improves, Rose recommends adding simple cognitive tasks while performing easy balance tasks. Examples include:
- Standing in a reduced base of support (such as feet together) while counting backwards by three’s, tossing an object from hand to hand, or saying as many words as possible that begin with the letter C
- Walking while counting backwards but without reducing your speed
“Keep in mind that the more cognitive effort required to perform each task, the worse your performance is likely to be on one or both tasks,” says Rose. “This is why you need to achieve a level of processing automatically on one task (preferably balance) so that attention can be allocated to the second cognitive task more easily.”
“We didn’t measure falls in our study,” says Jones, “but the assumption is that as balance improves, the risk of falling should be reduced as well.”
Related Symptoms
Sensory Sensitivities – Ear-related symptoms like tinnitus (ringing or swooshing sounds), dizziness, and vertigo are common. Eye-related symptoms like photophobia (sensitivity to brightness) also occur.
Fibrofog – Cognitive impairments involve a whole spectrum of difficulties, including auditory and visual, that can interfere with your processing of sensory inputs.
Treating Fatigue – Patients display more severe balance deficits when they are more fatigued.
Altered Metabolism – Fibromyalgia messes with your metabolism, causing you to be prone to weight gain and more susceptible to falling.
Yoga and Tai Chi – Both of these therapies may improve your balance. Helpful YouTube videos are available on the hyperlinked page (scroll down to bottom of that page for the videos).
Research holds the key to a better life. AFSA funded six projects in 2024 and 2025. We hope to fund more in 2026 but need your support (we are a small group of volunteers trying to make a difference).
Don’t Miss a Beat on New Treatments & Research: Sign up for a Free Membership today.
Medications | Alternative Treatments | Finding a Physical Therapist | Muscle Pain Relief
References for Fibromyalgia Balance & Coordination
- Watson NF, et al. Arthritis Rheum 60(9):2839-2844, 2009. Free Report
- Jones KD, et al. J Clin Rheumatol 15(1):16-21, 2009. Free Report
- Perez-de-Heredia-Torres M, et al. Exp Brain Res 226:137-143, 2013. Abstract
- Jones KD, et al. Arthritis Res Ther 13:R127, 2011. Free Report
- Perez-de-Heredia-Torres M, et al. BMJ Open 7(7):e016239, 2017. Free Report
- Rutledge DN, et al. J Adv Nurs 6(2):435-448, 2012. Abstract
- Dabbous AO, et al. J Int Adv Otol 20(3):247-254, 2024. Free Report
- Mingorance JA, et al. Healthcare 9(11):1533, 2021. Free Report
- Rose DJ. FallProof! A Comprehensive Balance and Mobility Training Program. Champaign, IL: Human Kinetics, 2025.
